Hereditary/Acquired Bleeding Disorders

Section Editor
Jennifer Donkin, PNP, DNP
Children’s Hospital Los Angeles
Case Study
Management of Thrombosis in a Patient With Antiphospholipid Antibody Syndrome
Presentation and History
The patient, a 26-year-old female, has antiphospholipid antibody syndrome (APS) and a history (in 2010) of unprovoked right femoral deep vein thrombosis (DVT) with slow resolution and with mild symptoms of post-thrombotic syndrome. APS, a systemic autoimmune disorder, is marked by recurrent arterial or venous thrombosis, sometimes with pregnancy morbidity, in the presence of persistent antiphospholipid autoantibodies.
This patient has had some adherence issues with warfarin and experienced a new DVT or an extension of DVT of the right femoral vein, extending to the iliac vein. She presented with a DVT of the right lower extremity (RLE) on June 17, 2021.
Upon presentation, there is swelling and tension of the right calf and right thigh, and the patient states that her right thigh feels warm to the touch. She first noted symptoms 3 days prior to presentation and says they have worsened daily. Her symptoms initially led her to visit the emergency department (ED) of a local hospital, where ultrasound showed a DVT in the femoral vein extending to the iliac vein. At her local hospital, anticoagulant therapy with enoxaparin (Lovenox) was initiated.
Patient Evaluation
Seven days later, she presents to the hematology specialty clinic. Relevant laboratory and clinical findings include: BMI 36.4, BSA 1.98 m2, heart rate 87 bpm, BP 113/67, and Tmax 36.8. ENT, cardiovascular, respiratory, and gastrointestinal findings are normal, with no bleeding reported. Regarding genitourinary symptoms, the patient states that her menses are irregular, lasting 4 to 5 days. During menses, she experiences cramps and clots. She uses 3 to 4 pads per day, changing them when they are 50% saturated; she denies hematuria. Physical examination reveals no hematologic/lymphatic symptoms of note, and the patient did not have bruising. There are also no notable endocrine, allergy/immunologic, skin, neurologic, and psychiatric systems.
Her musculoskeletal assessment, as mentioned, is significant for chronic swelling of the RLE, which is swollen, warm, and slightly tender on palpation. The RLE has increased girth compared with the left lower extremity, but range of motion and strength are normal.
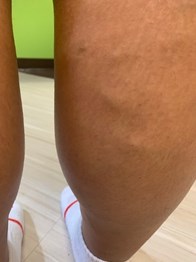
Imaging was performed due to the patient's history of DVT and increased swelling and pain of the RLE. Imaging revealed an extensive occlusive thrombus at the right external iliac and right common femoral vein extending towards the proximal femoral vein. (See Figure for clinical images of the patient's RLE.) The left common femoral vein was patent. Detailed assessment of the distal femoral vein was limited by body habitus.
Treatment Plan and Discussion
The patient's medication was previously changed from warfarin to apixaban (Elequis), an anticoagulant indicated for patients with a history of prior blood clots, about a year and a half prior. This change was due to warfarin contraindications in women who are or may become pregnant and the difficulty of monitoring warfarin INR [target international normalized ratio]. At this time, the patient was not willing to have an IUD placement which would have been preferred for pregnancy protection. However, at the hematology specialty center, her treatment was changed back to warfarin 3 months prior to the second DVT, because recent studies suggest that in patients with APS, warfarin is associated with a higher rate of thrombosis prevention.
Upon her presentation back to the specialty center once a new DVT was observed, the patient's anticoagulant therapy was changed from enoxaparin (which was started in the local ED) back to warfarin, at a dosage of 5 mg daily. Prothrombin time results were adjusted to the INR in 1 week and will be adjusted monthly if the regimen shows therapeutic efficacy. The goal range of INR to achieve basic anticoagulation is 2.0 to 3.0. An antiphospholipid antibody panel should be performed at the next clinic visit in 1 month and then every 6 months indefinitely.
Pregnancy counseling was again done regarding the birth defects risk associated with warfarin. The patient was not a candidate for birth control pills containing estrogen given their associated increased risk of thrombosis coupled with the thrombosis risk posed by her APS. She declined other options, such as an IUD, and stated that she is not currently in a sexual relationship. Further counseling and discussion in this area is warranted, however.
Physical therapy assessment was performed for accurate measurements. The patient has routinely worn a compression sock on her RLE to help with symptoms of post-thrombotic syndrome, a complication of DVT. At this time, she was encouraged to postpone wearing the sock secondary to changes in the girth of her RLE and acute thrombosis. This will be reassessed at the next clinic visit.
In addition, the healthcare team at the hematology specialty center conducted a psychological evaluation of the patient as well as a social worker evaluation and transition discussion. She is receiving ongoing wellness care from a primary care provider.
The most common cause of mortality from APS is thrombosis, which accounts for two-fifths of deaths. Evidence is emerging that chronic vasculopathy can occur in patients with APS even when they are taking anticoagulation therapy, and this is an area of future investigation. A recent review1 on the management of APS highlights current accepted anticoagulant therapies as well as other potential therapies (immunomodulating agents, statins, novel therapies including sirolimus and defibrotide) for patients with this rare disorder.
Reference
- Rodziewicz M, D'Cruz DP. An update on the management of antiphospholipid syndrome. Ther Adv Musculoskel Dis. 2020(12):1-10.
Figure. (A) Photograph of patient's right lower extremity (RLE), showing deep vein thrombosis (DVT) of the right external iliac and right common femoral vein extending towards proximal femoral vein. (B) Enlarged view of the patient's (RLE), showing DVT.
(A)
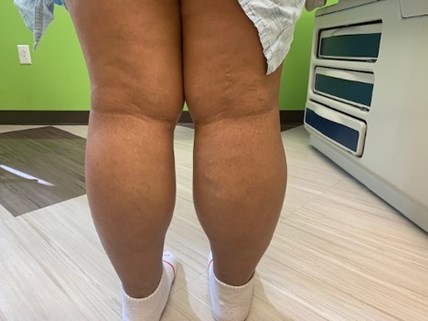
(B)